While every business should (still) be taking steps to avoid cross-contamination, it’s especially important for those who work with the young, ill, elderly or vulnerable, as well as those in residential or ‘communal’ settings who can play a key role in containing and preventing the wider spread of infectious diseases or viruses.
Read on to check our top infection control tips, and give your business the best chance of successful outbreak prevention.
Infection control is governed by lots of laws, Acts and regulations – such as the Health & Safety at Work Act 1974, The Public Health (Infectious Diseases) Regulations 1988 and the Health and Social Care Act 2008. Up-to-date advice can be found via the GOV.Uk websites – the British Geriatric Society also provide useful information regarding the COVid-19 outbreak.
Infection control responsibilities
As employers and employees we all have a duty of care – our responsibilities in terms of health and safety and the control of infections are summarised below:
Employers must:
- Assess the risk of exposure to infections
- Decide what controls and measures are needed to eliminate or reduce the risks
- Put infection control procedures and processes in place to carry them out
- Make sure the controls work and are used
- Provide suitable personal protective equipment (PPE)
- Provide regular training and information
- Ensure a clean working environment
Employees must:
- Take care of their own health and safety, as well as that of others
- Co-operate with their employer on safety matters
- Know and use any control measures including personal protective equipment (PPE)
- Follow safe systems of work
- Co-operate with policies and procedures
- Abide by local rules
- Report hazards and potential risks
An infection outbreak can be defined as:
Two or more people with the same infection caused by the same organism who probably acquired the organism in the same place
Or
More people than you would expect with the same infection.
Source: Public Health England (2014)
Infection control tips
1. Wash your hands thoroughly
Step 1: Prepare
- Wet your hands with warm water (ideally between 35 and 45 degrees)
- Completely cover your hands (including your thumbs) with soap and make a lather. Ensure soap covers the whole of each hand
Step 2: Wash
- Using your right palm, rub the back of your left hand, ‘locking’ your fingers as you go to ensure soap gets to the hard-to-reach areas – and repeat on your right hand
- Then, rub your palms together – again with fingers interlaced – and rub the back of your fingers (both hands)
- Twist your left thumb with your right hand, and vice versa
- Rub your left palm with clasped right fingers, and vice versa
- Rub your left wrist with your right hand, and vice versa
Important: Wash your hands for at least 20 seconds every time
Step 3: Rinse & Dry
- Thoroughly rinse both hands until all soap is gone
- Dry well – ideally using a hand dryer or disposable towel
It’s especially important to wash hands (and arms if necessary) before and after touching your eyes, nose or mouth. You should also wash before and after eating, drinking, smoking, taking medicine, applying make-up and handling contact lenses – and maintain good hand hygiene by using tissues and avoiding touching your face.
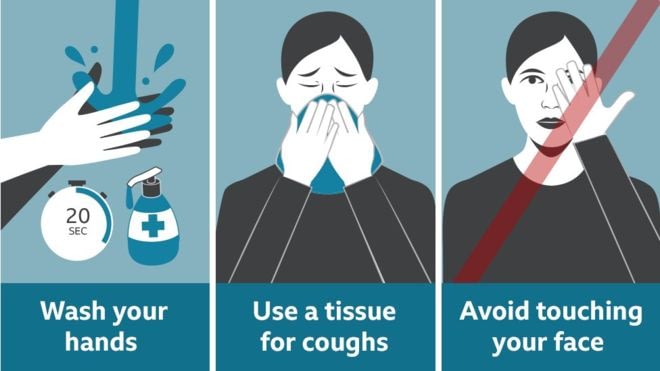
Image courtesy of bbc.co.uk
Working in care?
If you work in a care or healthcare setting, there are five important ‘hand hygiene moments’ according to the World Health Organisation (WHO):
- Just before you provide care to a resident
- As soon as you have finished providing care to a resident
- Straight after you have been exposed to any body fluids
- Straight after touching the person’s surroundings (e.g. chair, door handle)
- As soon as you take off protective gloves
In addition to the hand-washing guidelines above, it’s important that care workers also keep arms bare below the elbow, remove wrist and hand jewelry, maintain short, clean fingernails without nail polish or false nails and cover cuts or grazes with a waterproof dressing.
2. Be more aware of cross-contamination
Lift buttons, bannisters, conference calling devices, water coolers – and of course the handles and poles on public transport on our commute are all things we don’t normally think twice about touching throughout the working day (or night) – but being vigilant when using all of the above plays a huge part in infection prevention.
While avoiding them completely might not be practical, it’s important to use hand sanitiser – or ideally wash our hands with soap and water – as soon as possible after contact. Some viruses can survive up to weeks after being spread onto surfaces, so taking measures to avoid transferring them to other things we touch every day will help prevent outbreaks and break the chain of infection.
JLA Ultra Pearlised Hand Soap
Maintain good personal hygiene across your premises
Useful in any commercial environment, the JLA Ultra Pearlised Hand Soap is kind to skin while still being tough on grease and dirt.
3. Clean all rooms thoroughly and regularly
You should clean areas that are prone to infectious bacteria contact regularly, including residents’ and patients’ rooms, toilets, bathrooms, sluice rooms, receptions and waiting or common areas.
The disinfectant process should not create infectious aerosols (steer clear of water sprays). Good practice is to spray directly onto the cloth and then wipe over the surface. Change your cleaning cloths regularly and laundered these as infected linen or use disposable. Pay particular attention to communal areas where contact surfaces will be high risk – this may include stair rails, door handles etc.
If possible, you should also use a portable room sanitiser that can eliminate harmful micro-organisms such as MRSA, Norovirus, E.Coli, Salmonella and C.difficile to give both smaller rooms and communal areas an enhanced clean – providing additional reassurance that all surfaces even those inaccessible to manual cleaning will be disinfected.
Instead of choosing a filter, ioniser or spray which will only mask smells without eradicating harmful bacteria, look for models that use natural disinfectants like ozone, which can neutralise unpleasant odours and leave a ‘fresh after a storm’ fragrance at the same time as disinfecting.
JLA Sanitiser
The ultimate deep clean machine
The JLA Sanitiser eliminates harmful micro-organisms such as MRSA, Norovirus, E.Coli, Salmonella and C.difficile and neutralises unpleasant odours.
Instead of choosing a filter, ioniser or spray which will only mask smells without eradicating harmful bacteria, look for models that use natural disinfectants like ozone, which can neutralise unpleasant odours and leave a ‘fresh after a storm’ fragrance.

4. Make sure your laundry process is ‘infection control’ compliant
While effective infection control is of course something all on-premise laundry rooms should strive to achieve, formal guidelines only tend to be set for certain types of business like care/nursing homes and hospitals. However, these are equally important in other industries such as food and the hospitality markets.
Here’s a quick overview of three key points that cover how businesses like care and nursing homes are advised to achieve the correct handling of laundry to prevent spread of infection by the Department of Health:
- Laundered items to be stored in a clean area, above floor level
- Laundry area should be designed to minimise recontamination with good segregation between dirty (laundry recieipt) and clean areas
- Manual sluicing should be avoided in the laundry room under all circumstances
For guidance during the Covid19 outbreak, GOV.uk have released documents to assist those providing services in the social care sector. JLA have also produced a handy list of the key points of laundry infection control best practice and procedures.
The recommended thermal wash temperature process for fouled and infected linen is either 65 °C for 18 minutes or 71°C for11 minutes. Further clarification of the requirements for healthcare linen decontamination can be found in the Department of Health’s HTM01-04 guidance document. This also provides guidance and clarification of alternative laundry disinfection processes such as chemical and thermo-chemical disinfection. These should provide the same if not greater disinfection efficacy as thermal.
An alternative to thermal disinfection is the ozone washer system, which uses in situ generated O3 gas at low temperatures instead of high heat or chemicals that can damage garments and linen fabrics. Harnessing the natural power of ozone, this innovative way of washing kills bacteria, moulds, yeasts and viruses and reduces the risk of cross-infection in laundry.
5. Run a First Aid refresher
Cuts and grazes pose a particularly high risk when it comes to the spread of infection, as they’re a bloodstream entry point for viruses and bacteria – and blood or other fluids can in turn pass infections on to surfaces as well as directly other people.
You probably have good First Aid procedures in place, but when was the last time all staff in your business went through a ‘refresher’ – especially on day-to-day measures such as properly dressing and sanitising wounds?
6. Review your medical/sanitary waste disposal methods
You may manage facilities or work in a hospital, nursing home or care home where battling healthcare associated infection is a constant challenge. If so, it’s vital to redouble your efforts when it comes to safely disposing of healthcare waste which can spread infection, such as dressings and disposable clothing or sanitary items.
JLA Macerators
Automate your sanitary and waste disposal process
Macerators can be a good investment here, removing the need to use yellow bags for waste, and reducing the risk of ‘wide area’ cross-contamination that comes from handling and transporting waste throughout different rooms and communal areas.
JLA’s range of macerators offer a fast, hassle-free alternative to manual apparatus – and eliminate the risk of wide area contamination that can occur when using yellow bags.

7. Re-evaluate your food hygiene processes
There are a number of things to consider when it comes to maintaining high standards of infection control in relation to food hygiene in your business – including the Food Safety Act, dishwashing, HACCP guidelines, storage and preparation and CQC inspection ratings.
Along with laundry and room/surface disinfection, you should always seek expert advice for a dedicated commercial catering process that includes the right equipment, the right layouts and the right plans for staff to follow to keep cross-contamination, and ultimately a disease outbreak, at bay.
Our commercial laundry, hygiene and catering consultants will be happy to talk through your concerns, offer expert advice on compliance, and tailor solutions to specific challenges you might be facing.

Helen Buchan, Infection control expert
Helen is Head of Product at JLA and specialises in infection prevention and compliance. Drawing on nine years’ experience, she oversees the development, testing and deployment of infection control solutions for high-care environments, including care homes and hospitals.
With deep expertise in product research and development, Helen has developed a detailed understanding of both healthcare regulations and our customers’ challenges. This makes her an important bridge between science, compliance, and real-world performance.
Crucially, Helen translates her technical knowledge into clear, actionable guidance. Across the UK and Ireland, her work supports safer practices while helping organisations reduce their carbon impact and operating costs, without compromising hygiene or care standards.
Awards and accreditations
• Panel member for BIM4Housing
• Nominee for Influencer of the Year at the Women in Fire Safety Awards 2023
• Won the Spirt of JLA Award 2022

